Photos Cameron Flaisch and Jason Huynh
Teresa Resch was tired of living in pain.
An active 57-year-old from Rome, Ga., Resch wasn’t able to do many of the things she enjoyed. Gardening, playing with her grandkids and even sleeping had become too painful.
Seven months prior, Resch had slipped in the shower. As she fell, her hand shot out to catch herself, but her body hit the floor. Her arm had stayed where it was, and she tore her rotator cuff and biceps tendon.
“I tried physical therapy, taking anti-inflammatory drugs, and alternating heat and ice,” she says. “I wasn’t sleeping at night.”
Resch went to visit Harbin Clinic Orthopedics & Sports Medicine Rome, where she became a patient of Dr. Brad Bushnell.
After reviewing her case, Dr. Bushnell saw that she qualified for a new type of device he’d been using to help repair rotator cuff tears. Dr. Bushnell had been enrolling patients into a post-market medical research study for the REGENETEN™ Bioinductive Implant – and he had been getting amazing results.
“For me, surgery was the last resort,” says Resch. “But I felt confident after talking with Dr. Bushnell. Having gone through seven months of pain, inability to function well and not sleeping, I felt like surgery was my only choice.”
As it turns out, the rotator cuff surgery with the implant was one of the best choices Resch ever made for her health.
“I had great results. I have absolute full motion of my arm in every direction,” says Resch. “I can lift things with no trouble, I’m sleeping well. I think I did great.”
The way Dr. Bushnell initially came across the Regeneten implant was serendipitous.
“I was at a sports medicine convention in Seattle in 2014 and I ran into an old friend while I was in a line to get coffee,” says Dr. Bushnell. “He used to work for one of the big orthopedic companies, but had just taken a new job with a start-up business. He said, ‘Hey man, it’s good to see you. You got a minute?’ And the rest is history.”
At first, the effectiveness of the implant seemed too good to be true, but Dr. Bushnell saw rapid and convincing results. He and Clinical Research Coordinator Terri Brannon have diligently tracked data on a multitude of patients and contributed to several published multi-center research papers about the implant. Overall, he has completed more than 160 surgeries with it.
Resch was a participant in one of the studies, which encouraged her throughout her healing process.
“I’d never been part of doing research for a medical procedure and it made me really want to be a good patient,” she says. “I made sure I followed all the instructions during recovery. I had a positive attitude, and I think that also makes a huge difference. If you don’t have a positive attitude, you have a tendency not to do what you’re supposed to do to get well.”
“The use of implants during rotator cuff surgery isn’t new,” says Dr. Bushnell, “but with this implant, they got the biology right.”
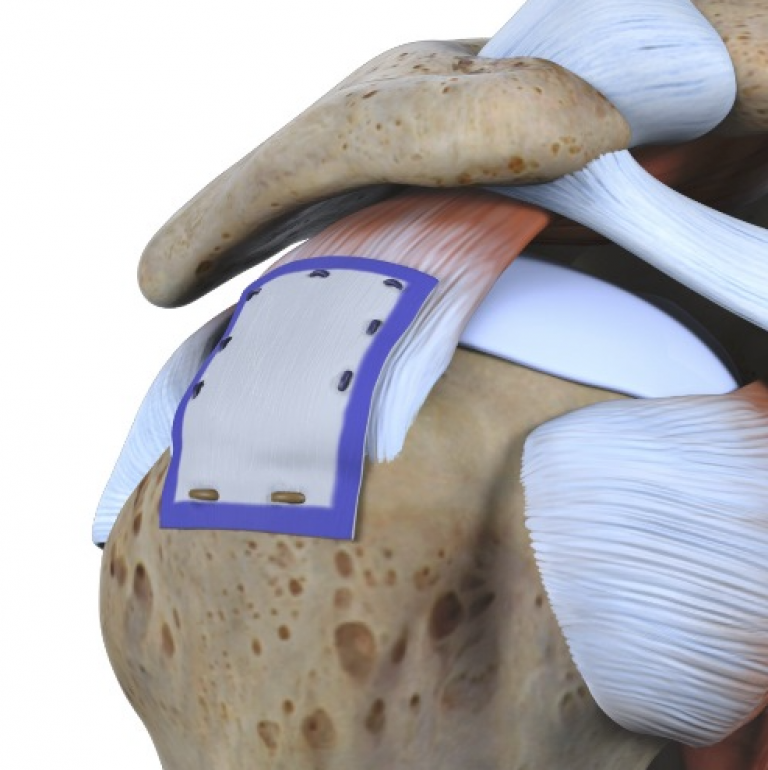
What makes the Regeneten Bioinductive implant especially attractive is that it hasn’t been shown to cause adverse effects for the patient. In previous cases, some implants could cause the body to have an allergic reaction, but this one doesn’t seem to do that.
“Another really innovative part is how quickly we can deploy it,” says Dr. Bushnell. “Some of the older implants used to require a big incision and a lot of time, but the delivery of this one literally takes me about two to three minutes using our standard small incisions.”
The implant is a patch about the size of a postage stamp and is created from the bovine Achilles tendons from a herd of cattle in New Zealand. The surgery is minimally invasive; Dr. Bushnell makes a small incision over the tear, then inserts and attaches the implant. It integrates biologically into the injured tendon and accelerates healing and strengthening.
“Imagine a rope holding up a weight,” says Dr. Bushnell. “Using the implant is like adding supplemental fibers to the existing rope. It’s not adding another rope, but more like wrapping something around the rope that makes it grow stronger.”
Tears occur from trauma, stress or general wearing of the tendon over time, and the implant helps with management and the protection of tendon injuries without a huge loss of tissue. Dr. Bushnell has found success in treating both partial and full tears with the implant.
“It seems to speed up healing of all types of tears,” he says. “However, the best results are in the partial tears where the rotator cuff is thinned out – it’s not ripped all the way off yet, but it’s getting there.”
Glenn Keaton, a painter and construction worker from Menlo, has had two rotator cuff surgeries. The first he had years ago without the implant.
“They went in and pulled the tendon out from under my shoulder and tied it down on the bone,” says Keaton. “I recovered from that, but it was pretty brutal. I was out of work for a good while.”
Once he was able to work again, Keaton had another accident and tore the cuff on his other shoulder. During this surgery, the tear was almost identical to his last injury – but this time, Dr. Bushnell used the implant.
“My recovery time was half of what it was before,” says Keaton. “Four days after my surgery, I painted 400 feet of picket fence. It’s like it cut my recovery time in half.”
The same was true for Zac Sanders of Cave Spring who had a partial rotator cuff tear, and his livelihood was at stake regarding his lawn care business.
“I told Dr. Bushnell, ‘If I don’t work, I don’t get paid.’ and Dr. Bushnell told me to give him about a week after my surgery. Well, a week and a half after having rotator cuff surgery, I went back to work,” says Sanders.
Both types of rotator cuff surgery – with and without the implant – work well in the long run. But the implant may be more effective in allowing people to get back to their lives, sooner.
“I have full range of motion; I can run my arm up my backbone,” says Keaton. “I could not be happier, but to tell you the truth, I can’t tell the difference between the right and left shoulder at this point. They’re both perfect.”
Dr. Bushnell also has additional tools to assist patients in their recovery after surgery.
“In many cases, the rotator cuff tear is not the only thing they have going on, medically,” says Dr. Bushnell. “There may be some bicep problems, cartilage issues, arthritis, bone spurs and other things going on in the shoulder that may change their rehab protocol. Although Regeneten has a standardized physical therapy protocol, we sometimes tweak it to provide a customized experience for each patient.”
Michael La Grange is another patient who was enrolled in the study. He explained that Dr. Bushnell had some home therapy equipment delivered directly to his house, and it was easy to use.
“One therapy aid was a chilling pad that fit over my shoulder and pumped icy cold water over it,” he says. “The cold was the best relief for pain. It felt so good to have the cold on there.”
There was also a chair-based machine that helped him stretch and move his shoulder.
“It has an arm that would gradually raise up and go down again,” says La Grange. “I used it within two weeks of surgery which definitely expedited the recovery process. It put me that much more ahead of things when I went to physical therapy.”
La Grange owns a farm and was also a wine merchant at the time of his surgery in 2015. He believes general overuse led to his second tear.
“When I had my right shoulder operated on years before, I spent the first two weeks in a recliner because there was no way I could lay down in bed with my shoulder,” he recalls. “After Dr. Bushnell did my rotator cuff surgery with the implant, I slept in my bed the first night home. I was out of my sling within 10 days. Each injury is different, each person is different, but my recovery from this surgery was just so much quicker.”
Now fully recovered, La Grange has nothing but great things to say about Dr. Bushnell and his team at Harbin Clinic.
“He’s a great person,” says La Grange. “He’s very frank and honest and has a good sense of humor. Dr. Bushnell was super responsive and so were the staff across the board. The teamwork and the care was excellent.”
One of the reasons Dr. Bushnell is the national leader in enrollment in the Regeneten patient registry is because he’s determined to prove it really works so more insurance companies will cover it.
“It’s a shame the implant isn’t available to everyone who needs it. One of my biggest hopes is that we can get this covered for more patients. If our research can really prove clinical benefits with cost effectiveness, we can make it happen. There are new studies starting up this spring, and some of my partners are now participating as well. It’s an exciting time.”
The cost-effectiveness factor includes that the surgery may reduce or eliminate the need for revision surgeries, prolonged physical therapy and the patient’s time out of work.
“I want it to be available for everyone,” he says simply. “It works.”
As far as his research goes, Dr. Bushnell says he’s thrilled that Harbin Clinic can be a national leader in orthopedic shoulder research.
“It’s wonderful that our numbers have outpaced those of our collaborators at places like Princeton and the Steadman-Hawkins Clinic in Denver. It’s a little friendly competition among national colleagues that goes a long way,” he says. “By providing care for our local patients and doing these research studies, we’re helping thousands of people out there we will never meet, in places that have never heard of Rome, Georgia. That’s pretty cool.”